How Wearing Compression Socks Can Help You at Work

When it comes to working long hours, whether at a desk or on your feet, wearing compression socks has become increasingly recognized as a proactive health measure. Prolonged sitting can reduce blood flow to the legs, potentially leading to blood clots. Standing for extended periods places extra strain on the circulatory system and can cause fatigue and soreness. Jobs requiring extended standing, such as nurses, retail workers, flight attendants, and restaurant staff, benefit from the all-day support provided by compression socks. Similarly, office workers, administrative staff, and those in sedentary roles can protect their legs by wearing compression socks to alleviate fatigue and prevent swelling. The therapeutic pressure of compression socks can promote better circulation, reducing achiness and energizing the legs. If you work in an occupation that requires you to stand or sit for prolonged periods, it is suggested that you make an appointment with a podiatrist to discuss relief methods and other ways to promote circulation in your feet and legs, such as wearing compression socks.
While working on the feet, it is important to take the proper care of them. For more information about working on your feet, contact James Pak, DPM from California. Our doctor will treat your foot and ankle needs.
Working on Your Feet
Standing on your feet for long periods of time can cause stress and pain in your feet. Your whole body may experience change in terms of posture, back pain, bunions, callouses and or plantar warts. There are ways to avoid these conditions with proper foot care, smart choices and correct posture.
Positive Changes
Negative heeled shoe – Choosing this shoe type places the heel slightly lower than the ball of the foot. These are great for overall foot health. Find shoes that fit you correctly.
Go barefoot – Our feet were not designed to be enclosed for all hours of the day. Try to periodically expose your feet to air.
Eliminate Pain
Foot Exercises – Performing simple exercises, incorporating yoga and doing stretches are beneficial. This will allow increased blood flow to the area and muscles of the foot.
Achilles tendon – Stretching the foot out flat on the floor will relax the calf muscles and tendon. These exercises can be performed almost anywhere. Make sure you add these exercises to your daily regimen.
With a little bit of this information and knowing more about foot health, you will notice changes. Foot stretches and proper footwear will help with pain and prevent further issues.
If you have any questions please feel free to contact our office located in Anaheim, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How to Handle a Long Work Day on Your Feet
In 2014, the American Podiatric Medical Association surveyed 1,000 American adults and found that half of all respondents lived with foot pain. Fortunately, there are ways to avoid foot problems such as following a daily footcare routine and wearing proper footwear at work.
If you have a job that requires you to be on your feet, it is best that you do not wear flat sole shoes. Your heel should be slightly elevated (less than 2 inches, but at least ¼-inch) if you are going to be standing for a prolonged period. You should also make sure that the shoes you wear are not too small. Tight shoes may cut off circulation to your feet, which will result in pain and blisters. It is always best to purchase fitted shoes later in the day, because the feet tend to swell as the day progresses. It may also be helpful to buy shoes a half size larger if you plan on wearing custom orthotics or arch supports.
Your muscles may become stiff when you are constantly standing up. It is important to take breaks every hour to stretch and relax. One tip is to perform calf raises, because this exercise will help improve your circulation. To perform this stretch, you first need to stand on the edge of a step with your abdominal muscles pulled inward. You then need to grip the step with the balls of your feet with your heels hanging over the edge. Next, try to raise your heels above the step by a few inches while standing on your tiptoes; hold this pose for a second. You should then lower your heels back even to the platform. These calf raises should be done ten times for full effectiveness.
You should also take care of your feet while you are at home. One of the best ways to prepare your feet for a long day of work is to soak them in ice water. Doing so for 20 minutes will help fight the swelling and inflammation that results from being on your feet at work.
Nevertheless, if you are experiencing pain in your feet, you should seek help from your podiatrist. Your doctor will help treat any ailments you may have in addition to helping you prevent any other ailments from developing in the future.
Are Bunions Affecting Your Everyday Life?
Causes of Bunions May Be More Than Just Footwear

Bunions, those bony bumps that form at the base of the big toe, are a common foot ailment that can cause pain and discomfort. While many people associate bunions with wearing tight or ill-fitting shoes, the causes are often more complex than simply blaming your footwear choices. One of the primary contributors to bunions is genetics. If bunions run in your family, you may be genetically predisposed to developing them. In such cases, the way your foot bones are structured can make you more susceptible. Another significant factor is having improper foot biomechanics. If your feet roll inward excessively when you walk, termed overpronation, or if you have a flat foot arch, the increased stress on the joint at the base of the big toe can lead to bunion formation over time. While wearing tight shoes with a narrow toe box can exacerbate the problem, they generally are not the sole cause of bunions. If you have developed a bunion, it is strongly suggested that you speak with a podiatrist who can determine the cause and guide you toward the treatment method that is best for you.
If you are suffering from bunions, contact James Pak, DPM of California. Our doctor can provide the care you need to keep you pain-free and on your feet.
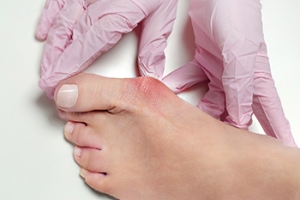
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
- Refrain from wearing heels or similar shoes that cause discomfort
- Select wider shoes that can provide more comfort and reduce pain
- Anti-inflammatory and pain management drugs
- Orthotics or foot inserts
- Surgery
If you have any questions, please feel free to contact our office located in Anaheim, CA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
Reducing Plantar Fasciitis Foot Pain

Plantar fasciitis is a common and painful condition that affects the heel and bottom of the foot. It occurs when the plantar fascia, a thick band of tissue that supports the arch of the foot, becomes inflamed or damaged. The pain from plantar fasciitis can be excruciating and debilitating, making simple tasks like walking a challenge. However, there are ways to reduce this pain and improve your quality of life. Included are stretching exercises for the calf muscles and Achilles tendon, custom or over-the-counter orthotic inserts to improve arch support and provide ample cushioning, and avoiding high heels and flip-flops. Other methods to decrease pain from plantar fasciitis are taking anti-inflammatory medications and using night splints to keep the foot in a dorsiflexed position, which helps stretch the plantar fascia during sleep. More advanced measures include corticosteroid injections to reduce inflammation and shockwave therapy, which stimulates healing in the plantar fascia. In rare cases, surgical intervention may be considered. If you are suffering from plantar fasciitis pain, it is suggested that you make an appointment with a podiatrist for treatment options that are right for you.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact James Pak, DPM from California. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Anaheim, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is the thick band of tissue that connects the heel bone to the toes. When this band of connective tissue becomes inflamed, plantar fasciitis occurs. Fortunately, this condition is treatable.
There are several factors that may put you at a greater risk for developing plantar fasciitis. One of the biggest factors is age; plantar fasciitis is common in those between the ages of 40 to 60. People who have jobs that require them to be on their feet are also likely to develop plantar fasciitis. This includes factory workers, teachers, and others who spend a large portion of their day walking around on hard surfaces. Another risk factor is obesity because excess weight can result in extra stress being placed on the plantar fascia.
People with plantar fasciitis often experience a stabbing pain in the heel area. This pain is usually at its worst in the morning, but can also be triggered by periods of standing or sitting. Plantar fasciitis may make it hard to run and walk. It may also make the foot feel stiff and sensitive, which consequently makes walking barefoot difficult.
Treatment for plantar fasciitis depends on the severity of the specific case of the condition. Ice massage applications may be used to reduce pain and inflammation. Physical therapy is often used to treat plantar fasciitis, and this may include stretching exercises. Another treatment option is anti-inflammatory medication, such as ibuprofen.
If you suspect that you have plantar fasciitis, meet with your podiatrist immediately. If left untreated, symptoms may lead to tearing and overstretching of the plantar fascia. The solution is early detection and treatment. Be sure to speak with your podiatrist if you are experiencing heel pain.
Foot Swelling During Pregnancy

Edema, the swelling or puffiness of body parts, can be a common discomfort during pregnancy. It typically affects the feet, ankles, and legs. This condition can also result in discomfort, potentially limiting the range of motion in your ankles. Edema occurs when excess fluid accumulates in the body's tissues. Several factors can contribute to this buildup, including gravity, diet, medication, and certain medical conditions. Fluid is naturally pulled down into your legs and feet, and sitting or standing for prolonged periods, especially in hot weather, can make swelling worse. Excessive amounts of salt can lead to fluid retention. Edema is not contagious, nor does it have a genetic predisposition. Regular exercise, such as walking, can aid in reducing edema by working the calf muscles, which assist in fluid circulation. It is also a good idea to elevate your legs as often as possible and wear some type of compression socks. Edema during pregnancy is a common occurrence, but it can be managed with lifestyle modifications and medical intervention. For more information on edema in the feet and ankles, it is suggested that you make an appointment with a podiatrist.
Pregnant women with swollen feet can be treated with a variety of different methods that are readily available. For more information about other cures for swollen feet during pregnancy, consult with James Pak, DPM from California. Our doctor will attend to all of your foot and ankle needs.
What Foot Problems Can Arise During Pregnancy?
One problem that can occur is overpronation, which occurs when the arch of the foot flattens and tends to roll inward. This can cause pain and discomfort in your heels while you’re walking or even just standing up, trying to support your baby.
Another problem is edema, or swelling in the extremities. This often affects the feet during pregnancy but tends to occur in the later stages.
How Can I Keep My Feet Healthy During Pregnancy?
- Wearing orthotics can provide extra support for the feet and help distribute weight evenly
- Minimize the amount of time spent walking barefoot
- Wear shoes with good arch support
- Wear shoes that allow for good circulation to the feet
- Elevate feet if you experience swelling
- Massage your feet
- Get regular, light exercise, such as walking, to promote blood circulation to the feet
If you have any questions please feel free to contact our office located in Anaheim, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Foot Care for Pregnant Women
The natural weight that pregnant women gain causes their center of gravity to be completely altered. This causes them to have a new weight-bearing stance which adds pressure to the knees and feet. As a result, pregnant women often experience severe foot pain. The two most common foot issues experienced by women in their pregnancies are edema and over-pronation. It is important for all pregnant women to learn more about how to take care of their feet so they are more comfortable during their pregnancy.
Over-pronation, which is commonly referred to as flat feet, is caused when a person’s arch flattens out upon weight bearing. This causes the person’s feet to roll inward while walking. Pregnant women often experience this due to the sudden weight they gain.
Edema, also referred as swelling in the feet, typically occurs in the later part of the pregnancy. It is the result of the extra blood accumulated in the pregnant woman’s body. The enlarged uterus puts more pressure on the blood vessels in the pelvis which causes leg circulation to slow down. This causes blood to pool in the lower extremities.
Fortunately, there are ways to treat both edema and over-pronation. Edema can be treated by elevating the foot as often as possible. Wearing proper fitting footwear will also be helpful for those with edema. A treatment method for over-pronation could be orthotics. Orthotic inserts should be designed with appropriate arch support and medial rear foot for your foot.
It is best for pregnant women to buy new shoes during the day, because this is the time where swelling is at its peak. Pregnant women also shouldn’t rush when buying shoes. It is always advised that you make sure your shoes fit properly but this is especially important during pregnancy.
If you are a pregnant woman, you should consult with a podiatrist in order to make sure your feet are healthy throughout the entirety of your pregnancy.
Symptoms of Charcot-Marie-Tooth Disease

Charcot-Marie-Tooth disease is a cluster of inherited genetic disorders that impact the peripheral nervous system. These neuropathies disrupt the intricate network responsible for movement and sensation within the extremities, including the feet. The peripheral nervous system serves as a communication bridge between the brain, spinal cord, and muscles. Charcot-Marie-Tooth disease results in a range of symptoms that interfere with this process and dramatically influence foot health. Gradual muscle wasting in the feet and legs is a hallmark of this disease, causing increasing weakness and reduced control over time. This frequently leads to difficulties in mobility and balance. It also can result in high foot arches, known as pes cavus, and clawed toes. These structural changes can further impede proper foot function and comfort. An altered gait, often high-stepping, and a slapping sound when walking are only some of the common symptoms. Poor balance and a risk of falling are others, caused by weakened muscles and loss of sensation. Although there is no cure, it is possible to manage foot-related challenges and potentially slow down the progression of the disease. For guidance, it is suggested that you make an appointment with a podiatrist.
When dealing with systemic disease of the feet, it is extremely important to check the affected areas routinely so that any additional problems are caught quickly. If you have any concerns about your feet and ankles contact James Pak, DPM from California. Our doctor will assist you with all of your podiatric needs.
Systemic Diseases of the Feet
Systemic diseases affect the whole body, and symptoms usually are displayed in the feet. This condition can make a patient’s ability to walk unbearable. Systemic diseases include gout, diabetes mellitus, neurological disorders, and arthritis.
Gout – is caused by an excess of uric acid in the body. Common symptoms include pain, inflammation, and redness at the metatarsal/phalangeal joint of the base big toe. Gout can be treated by NSAIDs to relieve pain and inflammation, and other drugs that lower the acid levels in the body.
Diabetes mellitus – is an increase in the level of blood sugar that the body cannot counteract with its own insulin. Failure to produce enough insulin is a factor in Diabetes.
Diabetes of the Feet
Diabetic Neuropathy – may lead to damaged nerves and affect the feet through numbness and loss of sensation.
Peripheral Vascular Disease – can restrict the blood flow to the feet, and often times lead to amputation of the feet.
If you have any questions please feel free to contact our office located in Anaheim, CA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.